| |
 Kidney Problems Kidney Problems
Select from the following topics to learn more about common Kidney Conditions.
Kidney Stones in Adults
Kidney stones, one of the most painful of the urologic disorders, are not a product of modern life. Scientists have found evidence of kidney stones in a 7,000-year-old Egyptian mummy. Unfortunately, kidney stones are one of the most common disorders of the urinary tract. In 2000, patients made 2.7 million visits to health care providers and more than 600,000 patients went to emergency rooms for kidney stone problems. Men tend to be affected more frequently than women.
Click here to read more about kidney stones in adults.
About the Kidneys 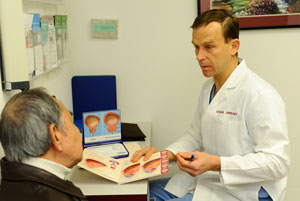
The kidneys are fist-sized, bean-shaped organs located near the middle of the back, just below the rib cage. Their primary function is to filter impurities and waste products from the bloodstream. Wastes removed by the kidneys are passed on to the bladder through tubes called ureters, where they are excreted in the form of urine.
The kidneys also produce three important hormones: erythropoitein (EPO), which triggers the production of red blood cells in bones; renin, which regulates blood pressure; and vitamin D, which helps regulate the body's calcium balance, necessary for healthy bones.
[Top] What Are Kidney Stones?
For reasons that are not completely understood, some of the substances in urine, uric acid and calcium in particular, may crystallize within the kidney, forming rock-like particles (calculi) called stones. The medical term for this condition is nephrolithiasis or renal stone disease. Kidney stones may be as small as a grain of sand or larger than a golf ball. Depending on their composition, they may be smooth, round, jagged, spiky or asymmetrical. Most stones are yellow to brown in color, although variations in chemical composition can produce stones that are tan, gold or black.
Some stones stay within the kidney, where they often produce no symptoms. Other stones may break loose and travel down the urinary tract. The smallest, smoothest stones may pass out of the body with little resistance and minimal discomfort to the patient. Larger, irregularly shaped stones cause intense pain. They also can become lodged in the ureter, bladder or urethra, the tube that carries urine from the bladder out of the body.
In addition to causing severe pain, a lodged stone can block the flow of urine, causing wastes to back up into the kidneys. Such a condition must be corrected swiftly, either by surgically removing the blocking stone or by nonsurgical medical procedures that break it up and allow it to pass naturally out of the body. If not, serious kidney damage and related medical problems can result.
[Top]
An estimated 600,000 persons in the United States develop kidney stones each year; of them about 100,000 are admitted to hospitals for treatment. Men are roughly four to five times more likely to develop the disease than women. It is generally estimated that 10% of men and 5% of women age 30 to 50 in this country will suffer from kidney stones. Most people who develop kidney stones experience their first episode between the ages of 20 and 30. The disease usually continues throughout life, particularly in men. Up to two-thirds of all men who have passed one stone will experience a recurrence, with an average of nine years between episodes. Kidney stones appear to be four to five times more common in whites than in African Americans.
[Top] 
No one is certain why people do or don't develop kidney stones. Although the disease appears to run in families, it is unclear whether this is associated with inherited physiological factors or merely the result of shared family dietary preferences that may predispose a person to stone formation.
Some researchers suggest the mineral composition of drinking water plays a factor, although they disagree as to whether "hard" (containing excessive calcium sulfate) or "soft" (excessive sodium carbonate) water is to blame. Alcohol consumption also may play a role in stone formation, particularly among drinkers who suffer from gout, a painful inflammation of the joints resulting from an imbalance in the body's uric acid metabolism.
Some experts, noting that residents of the southeastern United States have the highest incidence of kidney stones in the country, claim temperature and body dehydration are key factors. Others say the South's popular dietary staples of green vegetables, brewed tea and fatty foods are the cause.
Most scientists agree that eating specific foods by itself won't causes kidney stones. However, many experts acknowledge that certain diets, particularly those characterized by high-protein, salt, milk and animal fat intake may promote stone formation in people who are already susceptible to the disease.
Supersaturation
The most prevalent theory -- supersaturation crystallization -- holds that dehydration causes an imbalance in the liquids and dissolved solids in the urine. The kidneys must maintain a proper amount of water in the body as they remove harmful waste materials. If dehydration occurs, the urine may become overloaded (supersaturated) with substances that will not dissolve in water. These chemicals and trace elements combine to form crystals which slowly build up, layer upon layer until a stone is formed. Studies suggest that drinking plenty of water may prevent kidney stones.
Inhibitors
Normally, urine contains chemicals that prevent or inhibit the formation of crystals. Substances known to act as inhibitors include pyrophosphate, citrate, magnesium, zinc and macromolecules. Another prevalent theory holds that some persons do not possess these inhibitors in sufficient quantity to prevent crystallization, or that their inhibitors somehow fail to produce the necessary chemical reactions that prevent the formation of crystals. The formation of such crystals is the first stage in the development of a kidney stone.
Matrix
Another chemical component of urine, a noncrystalline mucoprotein called matrix, is thought by many experts to play a role in stone formation, although the precise nature of that role is still unclear. In persons who do not develop stones, matrix seems to act as an inhibitor. However, among patients who suffer from stones, matrix appears to be an initiator, and may even provide the chemical framework upon which crystals develop.
[Top]
Not all kidney stones are alike. Different types of chemical imbalances in the urine produce stones with different chemical compositions and varying shapes. The four most common types of stones are those made of calcium salts, struvite, uric acid and cystine.
About 70% to 80% of all kidney stones are composed of hard crystals of either calcium oxalate or insoluble phosphate salt, or a combination of both. Calcium stones are the most common type experienced by people of Anglo-Saxon descent. They occur in people who have hypercalciuria, a condition characterized by excessive calcium in the urine. Calcium is a normal part of a well-balanced diet, responsible for maintaining the health of teeth and bones. In most people, excess calcium is flushed out by the kidneys and excreted in the urine. People with hypercalciuria build up excess calcium in their kidneys, where it joins with other waste products to form a stone.
In about 40% of people who develop calcium stones, this buildup is caused by an inherited metabolic disorder whose cause is unknown. In rare cases, a tumor on the parathyroid gland may trigger an overproduction of parathyroid hormone, the chemical that regulates calcium metabolism. Certain drugs, such as the diuretic furosemide, antacids and steroids, can produce hypercalciuria. It also can be brought on by certain intestinal diseases, excessive amounts of vitamin A or D, or a diet too high in purine, typically associated with meat, fish and poultry consumption. Calcium oxalate stones also are commonly associated with having too little vitamin B or too much vitamin C in one's diet.
Uric acid is a normal byproduct made by the body as it breaks down protein. It is normally flushed out by the kidneys in urine. However, some people, particularly men, build up excessive uric acid concentrations in their kidneys or joints. In the joints, this can lead to gout, an inherited disorder of uric acid metabolism with painful arthritic symptoms. If this buildup occurs in the kidneys as well, it often results in the formation of uric acid stones.
An estimated 5% to 13% of patients with kidney stone disease, particularly men, develop uric acid stones. Genetics may play a role in uric acid stone propensity: Persons of Mediterranean descent, particularly those of Portuguese extraction, appear to have high incidences of uric acid stones, while those of Anglo-Saxon descent seem to be less at risk. Patients prone to developing uric acid stones typically are advised to reduce their consumption of high-protein foods, especially meat.
Also known as "infection stones," struvite stones account for up to 20% of all kidney stones. They are made up of crystallized magnesium and ammonia, common byproducts of excessive acidity in the urine caused by the bacterial breakdown of urea. This often occurs in persons who experience infections of the urinary system. For this reason they are most common in women, who suffer more urinary tract infections than men. Struvite stones typically develop in a jagged or branch-shaped structure called a "staghorn."
Cystine is one of the body's chemical building blocks, an amino acid that helps make up nerves, muscles and other body tissues. A rare genetic defect called cystinuria can cause excessive cystine buildup in the urine, leading to the development of cystine stones in the kidneys. Cystine stones are relatively rare, occurring in about 1% to 2% of persons who experience kidney stone disease. Because it is
genetically inherited, the condition often runs in families.
When a stone's location, size, shape and composition have been established, and any other medical complications such as infection or complicating diseases identified, the appropriate form of treatment must be determined.
Stone size is a major factor in determining how to proceed. Fortunately, most kidney stones, including many that become lodged on their way down the urinary tract, are less than 4 mm wide (about 3/16ths of an inch) and eventually will pass by themselves without the need for surgery or other active medical intervention.
[Top]
Expectant Treatment
If diagnostic procedures show a stone to be about 4 mm or less in diameter, and if the patient's symptoms aren't too severe, the doctor or urologist may recommend a course of expectant treatment or observation. This may take several weeks or even months, during which the patient will be advised to drink plenty of water -- up to three quarts a day, the equivalent of 8 to 10 large glasses -- to help flush out the stone and prevent others from forming. A change in diet also might be recommended.
Doctors often will recommend a second round of X-rays or ultrasound exams for expectant treatment patients one to two weeks after the stone is discovered to see if it is progressing down the urinary tract. If movement is detected, the treatment likely will be continued; if not, the patient's condition may be re-evaluated to determine if a more aggressive course of action is necessary.
Despite their discomfort, expectant treatment patients typically are advised to avoid becoming sedentary. Physical activity, especially walking, can help move a stone. However, kidney stone patients who are employed in jobs where a sudden attack of pain could place them in dangerous positions might be advised to stay home from work. Such jobs might include construction workers, drivers or heavy-equipment operators.
The use of a heating pad on a "low" setting, and/or over-the-counter pain medications like aspirin, acetaminophen or ibuprofen, may help relieve pain or discomfort while waiting for a stone to pass.
Patients who undergo expectant treatment typically are directed to strain their urine through a fine mesh strainer or thin cloth to catch the stone when it is passed and give it to their doctor for analysis. Many patients find it easier to urinate into a glass jar; the stone can be seen at the bottom of the jar. Catching the stone is important because analysis of its chemical composition can help the physician determine exactly what type of stone is being produced, which in turn suggests dietary and lifestyle changes to prevent future stone formation.
[Top]
Stone Extraction
If the stone cannot be passed spontaneously within a reasonable period --particularly if it is too large, produces excessive pain or bleeding, blocks the flow of urine, or causes acute ureteral colic or potential kidney damage -- some form of active treatment may be required to remove it. A variety of extraction methods, incorporating progressive levels of invasiveness, can be employed. Modern extraction procedures are greatly improved than those of only a few years ago and often result in much shorter recovery periods.
Ureteroscopy
Ureteroscopy is often the technique of choice with smaller stones that lodge in the mid- and lower sections of the ureter. It is a nonsurgical procedure in which a ureteroscope -- a flexible, fiberoptic instrument resembling a long, thin telescope -- is inserted through the urethra and bladder up to the stone. The urologist can then locate the stone visually and snare and remove it with a small cage or basket-like device inserted through the ureteroscope -- a procedure called endoscopic basket extraction. The doctor also may use a laser to crumble the stone into smaller pieces which can be passed by the patient. Ureteroscopy is performed under general or local anesthesia on an outpatient basis. Often the urologist will place a small silicone tube called a stent into the ureter for several days after treatment to relieve swelling and facilitate healing.
[Top]
Lithotripsy
Although kidney stones are quite hard -- particularly those formed from calcium -- a variety of nonsurgical techniques have been developed over the last 20 years to crush or pulverize them. Lithotripsy, a word of Greek origin meaning "stone-crushing," is one such method. It uses a machine called a lithotripter to project shock waves or sonic pulses against the stone and break it up. This can be done in several different ways, depending on the size and location of the stone.
The first lithotripters, developed in the early 1980s, were rather crude devices by modern standards and had to be used with great care to avoid damaging the patient's pelvis or kidneys. Nevertheless, they were able to break kidney stones into two or three pieces, which then could be manually extracted. The new generation of lithotripters are highly refined and capable of disintegrating stones into tiny particles that can pass out naturally with the patient's urine.
Typically, patients undergoing lithotripsy are given a sedative to help them relax and either a general or local anesthetic. Depending on the type of lithotripsy employed, the therapy may last over an hour, during which shock waves are focused on the kidney stone at a rate of approximately one per second. Some bruising may result from the shock waves, and discomfort may be experienced as the crushed calculi are passed, but most patients are able to resume normal activity in a few days.
Though highly effective for stones in the kidney and upper ureter, lithotripsy may not work for everyone. Occasionally, more than one treatment is needed to crush and pass all stone material. In rare cases, a catheter may need to be inserted through a small incision in the back to help drain the kidney and permit removal of stone fragments. Patients with very large stones or other complicating medical conditions may require a different form of treatment or surgery.
[Top]
Ultrasonic Lithotripsy
Similar to ureteroscopy, ultrasonic lithotripsy uses an optical scope and electronic probe, inserted into the ureter under epidural (spinal) anesthesia, to locate the stone. High-frequency ultrasound waves then are directed at the stone to break it up gradually. The fragments can either be passed naturally by the patient or removed by grasping forceps, basket extraction or suction through the scope instrument. The instrument is not flexible, however, so ultrasonic lithotripsy typically can be employed only when a straight path directly from outside the body to the stone is possible.
Electrohydraulic Lithotripsy (EHL)
This technique uses a special probe to break up small stones with shock waves generated by electricity. Through a flexible ureteroscope, the physician positions the tip of the probe 1 mm from the stone. Then, by means of a foot switch, the physician projects electrically generated hydraulic shock waves through an irrigating fluid at the stone until it is broken into small fragments. These can be passed by the patient or removed through the previously described extraction methods. EHL has some limitations: It requires general anesthesia, and is generally not used in close proximity to the kidney itself, as the shock waves can cause tissue damage. Fragments produced by the hydraulic shock also tend to scatter widely, making retrieval or extraction more difficult.
[Top]
Extracorporeal Shock Wave Lithotripsy (ESWL)
The most modern and frequently used outpatient procedure today for the removal of kidney stones, extracorporeal shock wave lithotripsy uses highly focused impulses projected from outside the body to pulverize kidney stones.
In its original form, ESWL treatment required the patient to receive sedatives and/or anesthesia and be suspended on a platform in a special water tank or bath. X-ray monitors were used to pinpoint the stone, which the lithotripter then bombarded with shock waves, breaking it into pieces which could be passed or extracted.
While a substantial improvement over other contemporary techniques and technologies, the early ESWL machines were less refined than those of today. They tended to produce more bruising and, because their first-generation design focused on patients of "average" height and weight, they didn't accommodate heavy, tall or small patients well. They worked well with stones located in the kidneys themselves or in the upper ureter, but were less effective at crushing stones in lower ureter.
Today's modern lithotripters, such as the Doli50, represent a high degree of development and design adaptation. They no longer require water baths; instead, the patient is positioned on a cushion atop a table. Without the need for a water tank, patient size restrictions are largely eliminated. Fewer X-rays are needed to establish the stone's position, and in most cases there is no need for general anesthesia; however, patients may be given medications to help them relax. The new-generation lithotripters also are much more effective at crushing cystine stones and those in the lower ureter than previous models. Treatment time is much shorter, and the stone usually is reduced to the consistency of sand, which typically can be passed normally in the patient's urine.
[Top]
Percutaneous Nephrolithotomy (PCN)
While ESWL is considered the state-of-the-art for treating most kidney stones, it still has its limits. Very large stones -- those 3 centimeters (about one inch) or more in diameter -- may require several ESWL treatments to break up completely, or may produce such a large volume of fragments when pulverized that they block the ureter. This condition is known as "steinstrasse," a German word meaning "street of stone."
Large struvite or "staghorn" stones, because of their jagged shape, sometimes become lodged in awkward positions or locations that make them difficult to treat effectively with shock waves.
ESWL also may be precluded if:
- The patient's kidney is already functioning poorly because of disease or defect and shock waves present an unacceptable risk of further damage
- The patient has a life-threatening heart problem or uses a cardiac pacemaker
- The patient is pregnant or suffers a bleeding disorder
- The size, location and number of stones would require excessive ESWL treatment
- The patient's kidneys or ureters are structurally abnormal or malformed
- The patient's symptoms are so acute that urgent treatment is necessary to prevent kidney damage
In such cases a different treatment involving some form of surgery, either alone or in combination with ESWL, may be required. Percutaneous nephrolithotomy (PCN) is one surgical option.
Percutaneous means "though the skin." In PCN, the surgeon or urologist makes a 1-centimeter incision under local anesthesia in the patient's back, through which an instrument called a nephroscope is passed directly into the kidney and, if necessary, the ureter. Smaller stones may be manually extracted. Large ones may need to be broken up with ultrasonic, electrohydraulic or laser-tipped probes before they can be extracted. A tube may be inserted into the kidney for drainage. The procedure usually requires hospitalization for several days, and most patients can resume normal activity within two weeks.
[Top]
Chemolysis
Certain types of kidney stones can be dissolved with the application chemicals. Uric acid stones, for example, can be dissolved with a solution of sodium bicarbonate in saline. Cystine stones may be treated successfully with a combination of acetylcysteine and sodium bicarbonate in saline. Struvite and carbon apatite stones can be treated with an acidic solution of hemiacidrin.
The procedure involves infusing the chemical solution into the affected area by means of a ureteral catheter in a series of treatments over time until the stone is dissolved. The patient's urine must be cultured regularly throughout the course of treatment to guard against urinary infection and prevent the buildup of excessive chemical levels, particularly magnesium, which can cause other health problems.
Chemolysis may be used as a primary form of treatment, or as an adjunct to percutaneous lithotripsy, surgical lithotomy or ESWL. Unfortunately, it does not work well with calcium stones, which are the most common type produced by persons with urinary stone disease.
[Top]
Open Nephrolithotomy
Usually reserved for the most complicated and difficult cases, open nephrolithotomy is the most invasive procedure for removing kidney stones. Because it is so traumatic, most kidneys can withstand no more than two such operations. Deep anesthesia is required, after which the surgeon makes a large (10-20 centimeter) incision in the patient's back or abdomen, depending upon where the stone is located. Either the ureter or the kidney is opened and the stone extracted. Most patients require prolonged hospitalization afterward, and recovery may take up to two months. [Top]
Partial Nephrectomy
Sometimes a kidney may be profoundly damaged by injury, disease or, in the case of kidney stones, serious infection or prolonged blockage. Big staghorn stones, which are produced by infection, often are involved in such cases. Whatever the cause, when a kidney's function drops below acceptable levels, radical surgery to remove all or part of the organ may be recommended. Nephrectomy means removal of the entire kidney. Partial nephrectomy, in which part of the kidney is removed, is rare, but may be appropriate if the damage, though profound, is confined to a portion of the organ.
[Top]
Recurrent Stone Disease Treatment
There are several forms of recurrent stone disease, each with its own particular underlying metabolic causes. Once testing has determined the type of stone a patient produces, the physician often can prescribe medication to help prevent the formation of new stones. These drugs control the chemical imbalances that lead to the formation of crystals in the urine -- the building blocks of kidney stones.
Hypercalciuria
Hypercalciuria, a condition characterized by excessive calcium in the urine and kidneys, is the primary cause of calcium stones, the most common type among people of Anglo-Saxon descent. There are three primary varieties of hypercalciuria.
- Resorptive Hypercalciuria
"Resorptive" means to dissolve and assimilate. Resorptive hypercalciuria is thought to be the result of a rare and incompletely
understood metabolic disorder which causes the body to produce too much parathyroid hormone (hyperparathyroidism), thus making the body dissolve its own bone tissue. The dissolved tissue creates excessive calcium levels in the blood, which then accumulate in the kidneys and produce calcium stones. In rare cases, the condition results from a tumor on the parathyroid gland. It also may be an inherited genetic condition. Other causes include cancerous tumors attached to bone tissue, myeloma (cancer of the bone marrow), Cushing's disease (a pituitary gland abnormality characterized by obesity and muscular weakness) and long-term immobilization, such as in paralyzed or bedridden persons.
- Treatment of Resorptive Hypercalciuria
Resorptive hypercalciuria produces recurrent stone formation regardless of dietary restriction. Treatment therefore consists of treating the underlying disorder that produces bone resorption.
[Top]
Absorptive Hypercalciuria
The most common form of hypercalciuria, this condition is found in more than half of patients with stones. It appears to result from an excessive intestinal response to vitamin D, making the body absorb too much calcium from ingested foods, typically meat, fish, poultry and dairy products. Certain drugs, such as the diuretic furosemide, antacids and steroids, also can produce absorptive hypercalciuria.
Treatment of Absorptive Hypercalciuria
Diet and Hydration
Patients suffering from absorptive hypercalciuria usually are placed on diets that restrict the intake of calcium and sodium. They are encouraged to add cereal bran to their diet because bran binds calcium in the gastrointestinal tract and helps excrete it from the body. Drinking 3-4 liters of water a day will reduce the patient's urinary calcium concentration and discourage the formation of urinary crystals.
Cellulose Phosphate
Another treatment for absorptive hypercalciuria is to add cellulose phosphate to the diet. This calcium-binding resin exchanges sodium for calcium in the gastrointestinal tract. However, because cellulose phosphate lowers magnesium levels in the blood and raises urinary oxalate levels, patients typically must take oral magnesium supplements and restrict their intake of oxalate-rich foods.
Orthophosphate
Adding orthophosphates to the diet helps absorptive hypercalciuria patients decrease their urinary excretion of calcium and increase their excretion of citrate and pyrophosphate, which in turn inhibits stone formation. Diarrhea is the most common side effect.
[Top]
Renal Hypercalciuria
About 1 in 10 cases of hypercalciuria are thought to result from an inability by the kidney to resorb calcium. As a result the patient's urine becomes overloaded with calcium. Restricting the patient's dietary calcium intake does not seem to decrease his or her urinary calcium, and adding calcium to the diet makes the condition worse.
Treatment of Renal Hypercalciuria
Doctors treat renal hypercalciuria with drugs called thiazide diuretics which increase the kidneys' resorption of calcium. Daily doses of hydrochlorothiazide usually are prescribed. Patients undergoing this therapy typically must supplement their dietary potassium intake and restrict their salt consumption. Patients who fail to respond to thiazide diuretics alone also may be given orthophosphates, with dietary calcium restrictions.
[Top]
Hyperuricosuria
Patients who form pure uric acid stones typically suffer from hyperuricosuria, a condition characterized by excessively acidic urine. About 25% of these patients have gout, an inherited metabolic disorder of uric acid metabolism with painful arthritic symptoms. Most patients with uric acid stones, however, simply seem to have highly acidic urine, perhaps exacerbated by dehydration, leading to supersaturation. Curiously, about 20% of patients with recurrent calcium stones also have hyperuricosuria, perhaps because the uric acid crystals provide a base upon which the calcium stones form.
Treatment of Hyperuricosuria
Patients with hyperuricosuria typically are advised to drink three liters of water a day to dilute the acidity of their urine. A daily dosage of 650 milligrams of bicarbonate of soda, the equivalent of two tablets, also is prescribed to neutralize the urine's acidity. This also may help dissolve the patient's stones. Patients on salt-restricted diets may be given potassium bicarbonate. If these measures fail to produce the desired result, dietary protein restrictions and use of a drug called allopurinol, which reduces uric acid excretion, may be prescribed.
[Top]
Hyperoxaluria
Hyperoxaluria is another disorder in which the body produces too much insoluble oxalic acid. The disease does not necessarily stem from excessive dietary oxalate intake, however. Instead, the cause appears to be related to some form of metabolic irregularity. There are three types of hyperoxaluria.
Primary Hyperoxaluria
A rare genetic disorder, primary hyperoxaluria leads to excessive buildup of calcium in the kidneys and soft tissue at an early age. Treatment consists of daily doses of the drug pyridoxine, which has been found to reduce oxalate excretion in some patients. Dietary oxalate restrictions -- limiting consumption of milk, eggs, ice cream, yogurt and cheese, tea or coffee, chocolate, peanuts, spinach, rhubarb and beets -- along with increasing fluid consumption may also be prescribed.
Enteric Hyperoxaluria
Patients with bowel disease and inflammation, or who have undergone small bowel bypass surgery, are likely to suffer from enteric hyperoxaluria, a condition in which large quantities of fatty acid in the bowel bind with calcium. This produces excessive oxalate which, when absorbed into the bloodstream, leads to the formation of calcium stones. A low-oxalate, low-fat diet with plenty of hydration and calcium supplementation is the prescribed form of treatment. The drug cholestryamine also can be used to bind oxalate in some patients.
Exogenous Hyperoxaluria
Another rare disorder, exogenous hyperoxaluria is caused when the body metabolizes substances ingested in large quantities to oxalate. Such substances include ethylene glycol (antifreeze), ascorbic acid (a vitamin found in citrus fruits, tomatoes, potatoes and green, leafy vegetables) and methoxyflurane, an anesthetic. Because the causes are environmental as well as dietary, treatment consists of preventing the patient from consuming the offending substances or restricting their dietary intake.
[Top]
Renal Tubular Acidosis (RTA)
RTA accounts for about 1% of calcium-based kidney stones. There are several forms of RTA, but the Type 1 disorder is primarily responsible for stone formation. In this condition, a defect in the kidney's distal tubule render it unable to maintain adequate hydrogen ion levels. This causes patients to form calcium phosphate, calcium oxalate or mixed stones. The prescribed treatment is to reduce the patient's urinary acidity with sodium bicarbonate or potassium citrate.
Unfortunately, passing a kidney stone or having one removed usually signals the beginning rather than the end of a person's experience with renal stone disease. The disease usually continues throughout life, particularly in men; and people who have had one stone are likely to develop another, especially if they have a family history of kidney stones. Unless they adopt a lifelong course of preventive treatment or change certain lifestyle habits, they run a substantial risk of recurrence within a year. About one-half to two-thirds of all men who have passed one stone will form another within 10 years; 80% of all patients have at least one more bout with the disease during their lifetimes. Doctors typically refer to such patients as "stone formers."
How Can Kidney Stones Be Prevented?
- Drink plenty of fluids.
Doctors in ancient Greece used to advise their kidney stone patients to increase their fluid consumption to "flush out the pipes and dilute the salts." Their advice is still good today.
Today's physicians agree that people in general, and stone formers in particular, should drink as much fluid, particularly water, as possible. This is especially true during hot weather and in warm climates. Doctors use the term hydration to describe this practice.
Drinking at least 7 to 12 large glasses of fluid, mostly water, throughout the day will increase the production of urine to at least two quarts a day. It also helps to prevent the urine from becoming concentrated with the crystals that lead to stone formation. A good habit to adopt is to drink an 8-ounce glass of water with each meal, between meals, before bed and during the night, if the patient wakes up to urinate.
The color of the patient's urine will tell if he or she is drinking enough. The less color, the better. Dark or bright yellow urine indicates high concentration, which is normal in the morning after a night's sleep, but bad if it occurs throughout the day. Proper hydration produces urine that is pale in color.
Additionally, because urinary tract infections are a primary cause of struvite stones, preventing these annoying and painful infections is always a good idea. Drinking plenty of fluid reduces the likelihood of such infection, and with it, the risk of staghorn stone formation.
- Consult a doctor or dietitian about calcium and oxalate in the diet.
If tests show the patient's urine to be high in calcium or oxalate, a change in dietary habits may be in order. It may be necessary to limit consumption of certain types of antacids and dairy products like milk, eggs, ice cream, yogurt and cheese, which contain calcium, as well as strong tea or coffee, chocolate, peanuts, spinach, rhubarb and beetroot, which are high in oxalate.
However, while eating a normal, well-balanced diet may help many stone formers, not everyone will benefit from a low-calcium diet. Some persons with high oxalate levels in their urine actually may be advised to increase their dietary calcium. Because each person is different, his or her dietary needs should be evaluated and adjusted as necessary in consultation with a qualified physician or dietitian. Furthermore, patients need to know why certain dietary changes will affect their risk of stone formation, and are more likely to make a lifelong commitment to these changes if they understand the reasons why they should be made.
- Eat meat only in moderation.
This is good advice for everyone, not just stone formers. The average American eats twice as much protein as he or she actually needs. In addition to reducing dietary fat and serum cholesterol, cutting down in animal protein reduces calcium intake and uric acid excretion. Some patients also may need to limit the amount of fish and poultry they eat as well, and increase their consumption of bran and other cereal fiber.
- Avoid excessive salt.
This is another good general dietary recommendation for everyone. In addition to promoting high blood pressure (hypertension), too much salt in one's diet increases urine calcium excretion.
What are kidney stones?
Kidney stones -- renal calculi (KAL-kyou-lye) -- are formed from chemicals in urine that crystallize and stick together. They can be small and pass painlessly from the kidney with the urine, or they can be large enough to become caught in the urinary system where they can cause severe pain. Kidney stones affect men four times as often as women, and the condition tends to recur.
What are the common causes of kidney stones?
No one is certain why people do or don't form kidney stones. Nevertheless, certain factors seem to contribute to their development. These include:
- Not drinking enough fluids, particularly water
- Chronic urinary tract infections (UTIs)
- Certain genetic and metabolic diseases
- Consuming certain foods/beverages in susceptible people
How can kidney stones be prevented?
Depending on the type of stone a person produces, there are several ways to reduce your risk of recurrent kidney stone disease.
- Drink plenty of fluids. Drinking at least 7 to 12 large glasses of fluid, particularly water, each day will increase the production of urine. It will also help to prevent the urine from becoming concentrated with the crystals that can lead to stone formation.
- Consult a doctor or dietician about the amount of calcium and oxalate in your diet. If tests show that your urine is high in either calcium or oxalate, it may be necessary to make certain adjustments to your diet.
- Eat meat in moderation. This is good advice for everyone, not just stone formers.
- Avoid excessive salt intake, which is another good general dietary recommendation for everyone.
- What foods and beverages contain calcium and oxalate?
If you are prone to forming calcium oxalate stones, your doctor may recommend that you reduce your consumption of the following foods/drinks:
- certain fruits, including apples, various berries, grapes, oranges, pineapples and figs
- vegetables including asparagus, beets, broccoli, collards, spinach, Swiss chard and turnips
- dairy products such as milk, cheese and ice cream
- beverages such as beer, wine, cola drinks, coffee, tea and cocoa
- black pepper, parsley
- yogurt, peanut butter and chocolate
Don't give up or avoid consuming any of these foods or beverages without first consulting your doctor. In many cases, you'll be able to eat or drink them in limited amounts.
What are the common symptoms of kidney stones?
Most often, the first symptom of a kidney stone is usually extreme pain. Typically, a person experiences a sharp pain starting in the back, at the waist, in the flank, stomach or groin. Nausea, vomiting, chills, fever and elevated blood pressure are common. Blood in the urine is another classic symptom of kidney stones. Other possible symptoms include burning and frequent urge to urinate, cloudy or foul-smelling urine, or a blocked urine flow.
How can I find out more information on kidney stones? Contact the organizations below:
- National Kidney and Urologic Diseases Information Clearinghouse
3 Information Way
Bethesda, MD 20892-3580
- American Foundation for Urologic Disease
300 West Pratt Street
Baltimore, MD 21201-2463
1-800-242-2383
www.afud.org
- National Kidney Foundation
30 East 33rd Street
New York, NY 10016
1-800-622-9010
www.kidney.org
- UrologyChannel
Kidney Stones
[Top]
Content reprinted with permission from Dialog Medical, DialogMedical.com and Neil Baum, MD, neilbaum.com.
Quick navigation links:
What is a Urology Center | Urologist | Urology Conditions | Urology Services | Resources for Health | Contact Urology Center in North Texas | Sitemap | Home
Disclaimer:
The pictures displayed in www.TexasUrology.com are images of actual patients and employees who have consented to have their picture in this website.

Website Design & Educational Content © Copyright 2023 MedIngenuity, LLC
Medingenuity develops content-rich educational web sites for urologists and urology group practices.
|
|